A 74-year-old man is brought to the emergency department after being involved in a major motor vehicle collision. According to the paramedics, the patient was a restrained passenger. The patient has superficial injuries to the lower extremities and blunt force trauma to the chest and abdomen. He has pain "all over" but is answering all questions appropriately. Blood pressure is 98/65 mm Hg, pulse is 105/min, and respirations are 21/min. Oxygen saturation is 100% on 40% oxygen via face mask. Examination shows bruising over the anterior chest and abdomen. Lungs are clear to auscultation. No murmurs or abnormal heart sounds are heard. The abdomen is soft, but diffusely tender to deep palpation. Which of the following is the best next step in evaluation of this patient?
Below is the code for an example image modal link
Flashcards
/* -- Un-comment the code below to show all parts of question -- */
| A. Bedside ultrasound examination (65%) | ||
| B. Cardiac biomarkers (1%) | ||
| C. CT scan of the chest and abdomen (31%) | ||
| D. Diagnostic peritoneal lavage (1%) | ||
| E.Noncontrast CT scan of the head (2%) |
Motor vehicle collisions are the most common cause of blunt thoracic and abdominal trauma. Blunt thoracic trauma resulting in blunt cardiac injury can manifest as a cardiac contusion leading to depressed cardiac contractility and acute heart failure; cardiac arrhythmias; or myocardial rupture leading to pericardial effusion, tamponade, and cardiogenic shock. Blunt trauma to the abdomen can result in sheering and compression of vasculature and internal organs (eg, spleen, liver) resulting in laceration, rupture, hemorrhage, and infarction.
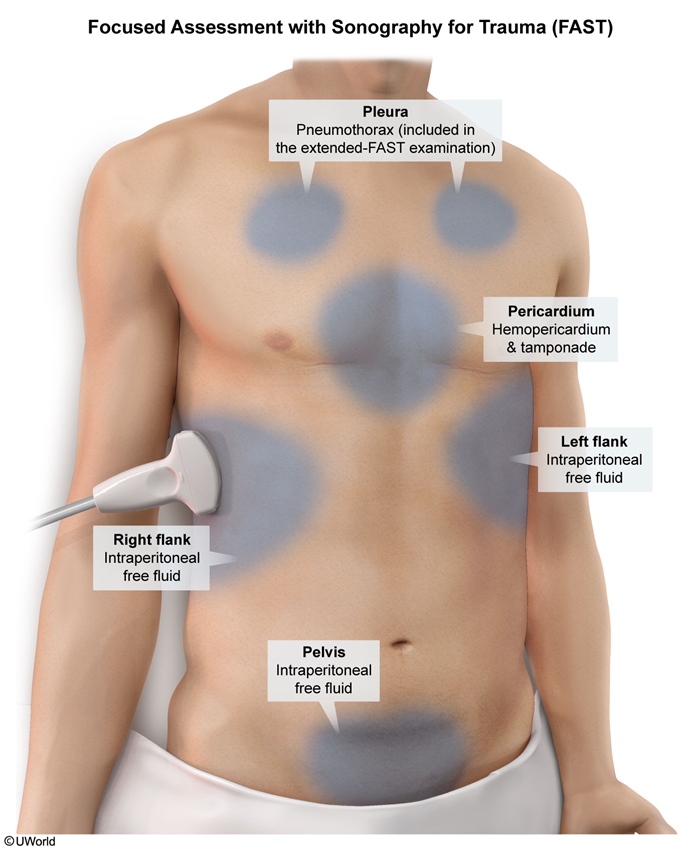
The diagnostic priority in patients with blunt thoracic or abdominal trauma and early signs of shock (eg, hypotension, tachycardia) is identification of rapidly fatal injuries (eg, pneumothorax, aortic dissection, pericardial effusion leading to tamponade, internal hemorrhage), which is best accomplished with bedside ultrasound or Focused Assessment with Sonography for Trauma (FAST) examination. Detection of abnormalities should prompt further directed evaluation (eg, CT scan, echocardiography) or specific therapy (eg, laparotomy, pericardiocentesis).
(Choice B) Cardiac biomarkers (eg, troponin I) are often elevated in patients with blunt thoracic trauma. However, the elevated levels are nonspecific, and routine measurement is not recommended unless there is high suspicion for myocardial infarction.
(Choice C) A CT scan of the chest and abdomen is often indicated in patients with blunt force injuries to the torso, however imaging is typically preceded by FAST to quickly assess for rapidly fatal injuries.
(Choice D) Diagnostic peritoneal lavage (DPL) is a rapid, highly sensitive procedure that can be used to evaluate for intraperitoneal hemorrhage. However, it is an invasive procedure, so is typically only performed in hemodynamically unstable patients when CT imaging and FAST examination are unavailable.
(Choice E) A noncontrast CT scan of the head should be obtained in patients with head trauma or abnormal neurologic findings suspicious for stroke. It is not indicated in this patient with injuries confined to the thorax, abdomen, and the lower extremities.
Educational objective:
Patients with blunt thoracic or abdominal trauma should have an initial screening with bedside ultrasound or focused assessment with sonography in trauma to assess for injuries that can be rapidly fatal (eg, pneumothorax, aortic dissection, pericardial effusion leading to tamponade, internal hemorrhage).